Potentiating Immunotherapy of Urological Cancers with Oncolytiic Viruses
Geertje van der Horst, Marjan van de Merbel, Thijs Janssen, Maaike van der Mark, Nadine van Montfoort, Rob Hoeben, gammaGabri van der Pluijm
Despite the promising effects of immunotherapy in other solid cancers, prostate cancer have remained largely unresponsive. In bladder cancer, immunotherapy has emerged as a promising therapeutic strategy but not all patients show clinically-desirable responses to immune-checkpoint inhibitors.
We hypothesize that oncolytic viruses (OVs) may unleash the full potential of cancer immunotherapy. OVs represent a promising therapeutic avenue, as OV-treatment combines tumour cell lysis with activation of the immune system and mounting of effective anti-tumour responses. For this, we evaluated and compared the oncolytic and immunostimulatory properties of multiple OVs , i.e. wildtype reovirus (R124) , a spontaneous mutant reovirus (jin‑3) and a new oncolytic derivative of the Gorilla-derived Human AdenoVirus‑B (HAdV-lumc007) ‘GoraVir’ in preclinical, ‘near-patient’ and syngeneic models of prostate and bladder cancer.
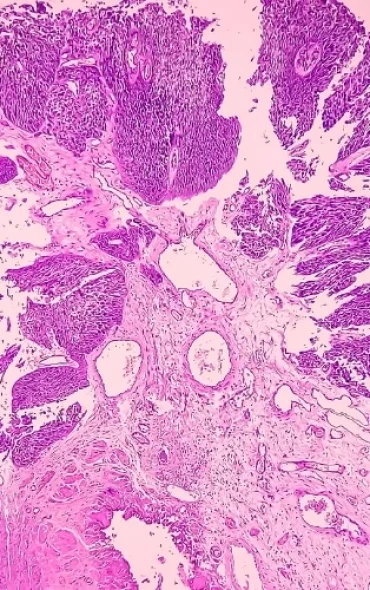
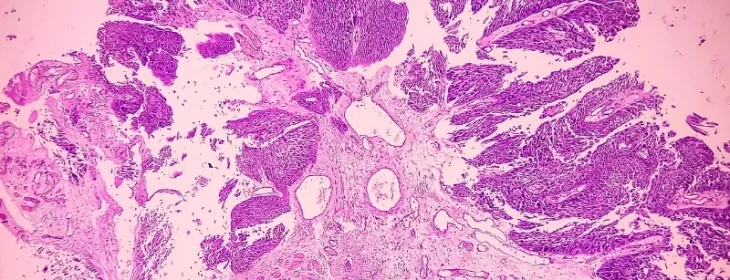
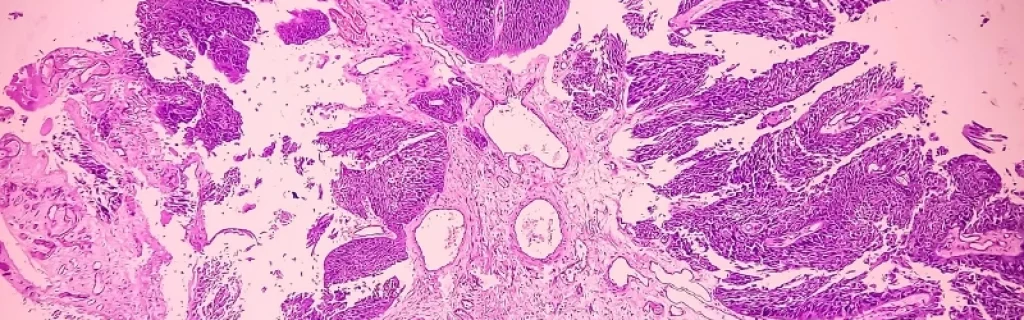
Both reoviruses variants and GoraVir effectively infected and lysed bladder and prostate cancer cells in 3D-cultures, ex-vivo cultured human tumour tissue slices and patient-derived xenograft (PDX) models. Notably, jin‑3 particularly, induces a dose-dependent expression of immunogenic cell death markers, interferon-stimulated genes and inflammatory cytokines.
Additionally, co-culturing reovirus- and to a lesser extent GoraVir- infected bladder and prostate tumouroids with peripheral blood monocytes resulted in a significant and dose-dependent cancer cell lysis and elevated production of CXCL10 and IFNgamma. Administration of jin‑3 to immunocompetent mice with a subcutaneously growing murine prostate cancer (TRAMP-C2) increased the infiltration of CD4+ and CD8+ effector cells in the tumour micro-environment resulting in tumor cell killing and cancer regression. Taken together, OVs elicit robust immuno-stimulatory responses highlighting their potential as anti-tumour agents.
Despite the promising effects of immunotherapy in other solid cancers, prostate cancer have remained largely unresponsive. In bladder cancer, immunotherapy has emerged as a promising therapeutic strategy but not all patients show clinically-desirable responses to immune-checkpoint inhibitors.
Show more
We hypothesize that oncolytic viruses (OVs) may unleash the full potential of cancer immunotherapy. OVs represent a promising therapeutic avenue, as OV-treatment combines tumour cell lysis with activation of the immune system and mounting of effective anti-tumour responses. For this, we evaluated and compared the oncolytic and immunostimulatory properties of multiple OVs , i.e. wildtype reovirus (R124) , a spontaneous mutant reovirus (jin‑3) and a new oncolytic derivative of the Gorilla-derived Human AdenoVirus‑B (HAdV-lumc007) ‘GoraVir’ in preclinical, ‘near-patient’ and syngeneic models of prostate and bladder cancer.
Both reoviruses variants and GoraVir effectively infected and lysed bladder and prostate cancer cells in 3D-cultures, ex-vivo cultured human tumour tissue slices and patient-derived xenograft (PDX) models. Notably, jin‑3 particularly, induces a dose-dependent expression of immunogenic cell death markers, interferon-stimulated genes and inflammatory cytokines.
Additionally, co-culturing reovirus- and to a lesser extent GoraVir- infected bladder and prostate tumouroids with peripheral blood monocytes resulted in a significant and dose-dependent cancer cell lysis and elevated production of CXCL10 and IFNgamma. Administration of jin‑3 to immunocompetent mice with a subcutaneously growing murine prostate cancer (TRAMP-C2) increased the infiltration of CD4+ and CD8+ effector cells in the tumour micro-environment resulting in tumor cell killing and cancer regression. Taken together, OVs elicit robust immuno-stimulatory responses highlighting their potential as anti-tumour agents.
Gabri van der Pluijm
Gabri van der Pluijm Ph.D. is Associate Professor at the Department of Urology, Leiden University Medical Center (Leiden, the Netherlands) at which he is heading the Urology Research Laboratory. His research is translational and ranges from 2D and 3D tumour-immune cell co-culture models in vitro to preclinical and ‘near-patient’ in vivo disease models for the study of the pathogenesis of tumour progression and experimental treatment of urological cancers (prostate, bladder and renal cancer).
His group is currently focussing on potentiating current immunotherapeutic approaches by oncolytic viruses and/or drug repurposing (cancer neuro-immunology), aiming at improving the treatment outcomes of patients with urological malignancies. Dr. van der Pluijm is (and has been) involved as coördinator and principal investigator in multiple national and international research consortia and research, including EU-sponsored European Training Networks. He is tutor of Medical and Biomedical Science students.
More about Associate Professor Gabri van der Pluijm.
Gabri van der Pluijm Ph.D. is Associate Professor at the Department of Urology, Leiden University Medical Center (Leiden, the Netherlands) at which he is heading the Urology Research Laboratory. His research is translational and ranges from 2D and 3D tumour-immune cell co-culture models in vitro to preclinical and ‘near-patient’ in vivo disease models for the study of the pathogenesis of tumour progression and experimental treatment of urological cancers (prostate, bladder and renal cancer).
Show more
His group is currently focussing on potentiating current immunotherapeutic approaches by oncolytic viruses and/or drug repurposing (cancer neuro-immunology), aiming at improving the treatment outcomes of patients with urological malignancies. Dr. van der Pluijm is (and has been) involved as coördinator and principal investigator in multiple national and international research consortia and research, including EU-sponsored European Training Networks. He is tutor of Medical and Biomedical Science students.

Read the Abstracts from Our Invited Speakers
Cancer Biology
- AllergoOncology: Lessons Learned from the Allergy-Glioblastoma Connection
Aurélie Poli, Luxembourg Institute of Health, LUXEMBOURG
- Cytotoxic NK Cells Impede Response to Checkpoint Immunotherapy in Melanoma with an Immune-Excluded Phenotype
Joanna Poźniak, KU Leuven, BELGIUM
- Inducing Immunogenic Tertiary Lymphoid Structures Across Cancer Types With Dendritic Cell Reprogramming
Camille Chatelain, Lund University, SWEDEN
- The Role of ILC2 in Tissue Homeostasis and Neoplasia
Tim Halim, Cancer Research UK Cambridge Institute, UNITED KINGDOM
Cancer Neuroscience
- Latent Neuropathy in Colorectal Cancer: Implications for Cancer Survivorship
Andrew Shepherd, University of Texas MD Anderson Cancer Center, USA
- Remodelling of the Bone Microenvironment During Cancer Infiltration: Insights from Multiplex Imaging and Spatial Transcriptomics
Christina Møller Andreasen, University of Southern Denmark, DENMARK
- Enteric Nervous System-Derived VIP Restrains Differentiation of LGR5+ Stem Cells Towards the Secretory Lineage Impeding Type 2 Immune Programs
Christoph Klose, Charité – Berlin University Medicine, GERMANY
Cancer Therapy
- Targeting the Dark Matter of Cancer with AI-Designed Mini Binder
Tobias Bald, University of Bonn, GERMANY
- Engineering Nanomedicines for Targeted Neuroimmune Modulation
Helena Florindo, University of Lisbon, PORTUGAL
- Potentiating Immunotherapy of Urological Cancers with Oncolytic Viruses
Gabri van der Pluijm, Leiden University Medical Center, THE NETHERLANDS
- Strategic Priorities in Cancer Therapy: Navigating the 2026 Cancer Mission Calls
Industry Contact Point, Łukasiewicz – PORT, POLAND
- Cancer Neuroscience of Brain TumorsKEYNOTE SPEAKER
Frank Winkler, Universitätsklinik Heidelberg, GERMANY
- Spatial Reprogramming of Immune Surveillance in Breast Cancer: From Immune Control to Immune Failure
Sheeba Irshad, King’s College London, UNITED KINGDOM
- The War Against Glioblastoma Needs More Than Standard of Care
Stefaan Van Gool, IOZK Immun-Onkologisches Zentrum Köln, GERMANY
- Uncovering the Spatial Regulation of γδ T Cells: Toward Receptor-Guided Immunotherapy
Jürgen Kuball, University Medical Center Utrecht, THE NETHERLANDS
- CAR‑T Cell Therapy in Lymphomas, Acute Lymphoblastic Leukemia, and Multiple Myeloma
Wojciech Szlasa, DCOPIH, POLAND
- Expanding CAR Targets to Non Protein Antigens
Sébastien Wälchli, Oslo University Hospital, NORWAY
- Advancing BIA-ALCL Research Through a UK – PORT Alliance — From Biobanking to Immune Discovery
Helen Kakkassery, King’s College London, UNITED KINGDOM
PORT for Business — Company Session
- From Sample to Insight: Advanced Analytics for Oncology Research
Malwina Woźniak, Łukasiewicz – PORT, POLAND
- Beyond glioblastoma — WPD Pharmaceuticals
Marek Sipowicz, WPD Pharmaceuticals, POLAND
- The Development of USP7 Inhibitor for Cancer Immunotherapy
Zbigniew Zasłona, Molecule, POLAND
- Leveraging Cancer Biology for Therapeutic Innovation: Clinical and Discovery Advances at Ryvu
Milena Mazan, Ryvu Therapeutics, POLAND
- Transforming Multimodal Complexity into Precision Oncology Insights
Marek Kudła, Ardigen, POLAND
- JJP-1008 as a Novel Checkpoint Inhibitor
Agata Drewniak-Maksymów, JPP Biologics, POLAND
- Synergistic Nanotechnology for Targeted Therapeutics in Oncology
Artur Wnorowski, Biotechna, POLAND
- Development of Biological Drugs for Oncological Indications at Mabion
Jakub Knurek, Mabion, POLAND
- Enabling Early Drug Discovery: Integrated Screening Capabilities and a BRD4/CRBN PROTAC Case Study
Justyna Adamczyk, Enamine, POLAND

